The most important muscle in your body is the heart, which pumps out the blood that keeps your tissues and organs nourished every day of your life. The largest blood vessel in the circulatory system is the aorta, and although it’s highly durable, sometimes its walls weaken and bulge, a phenomenon called an aortic aneurysm. If it ruptures, known as a dissection, the blood inside it will spill into your body and kill you.
Not all aneurysms burst. Some force blood to flow away from your tissues and organs, causing problems that range from heart attacks to kidney damage to stroke and even death.
Here at Prime Heart and Vascular, serving the greater Dallas, Texas area, Dr. Rashin Shah is a renowned cardiac and vascular specialist who’s triple board-certified, in Internal Medicine, Cardiovascular Medicine, and Interventional Cardiology. He specializes in both the diagnosis and treatment of the full spectrum of cardiac, peripheral artery, and venous diseases. He also believes that prevention of disease plays a more important role in staying healthy than is usually given credit.
What are the types of aortic aneurysms?
There are two types of aortic aneurysms: abdominal aortic and thoracic aortic.
1. Abdominal aortic aneurysms (AAA)
Sometimes referred to as “Triple A,” AAAs are located in the part of the aorta that passes through the abdominal cavity. They are the most common aortic aneurysms. Though a dilation of the blood vessel can be asymptomatic, when blood pressure increases to the point that the vessel ruptures, substantial internal bleeding results because of the aorta’s large size. Symptoms of a rupture include chest and jaw pain, difficulty breathing, a stabbing abdominal or back pain, and a weakness on one side of the body.
2. Thoracic aortic aneurysms
Thoracic aortic aneurysms develop in the part of the aorta that passes through the chest cavity. These aneurysms are also largely asymptomatic, so you may not know that you have one. However, a rupture may cause back pain, shortness of breath, and a tenderness or pain in the chest.
What are the risk factors for developing an aortic aneurysm?
Doctors aren’t certain what causes an abdominal aortic aneurysm, but the risk factors may include:
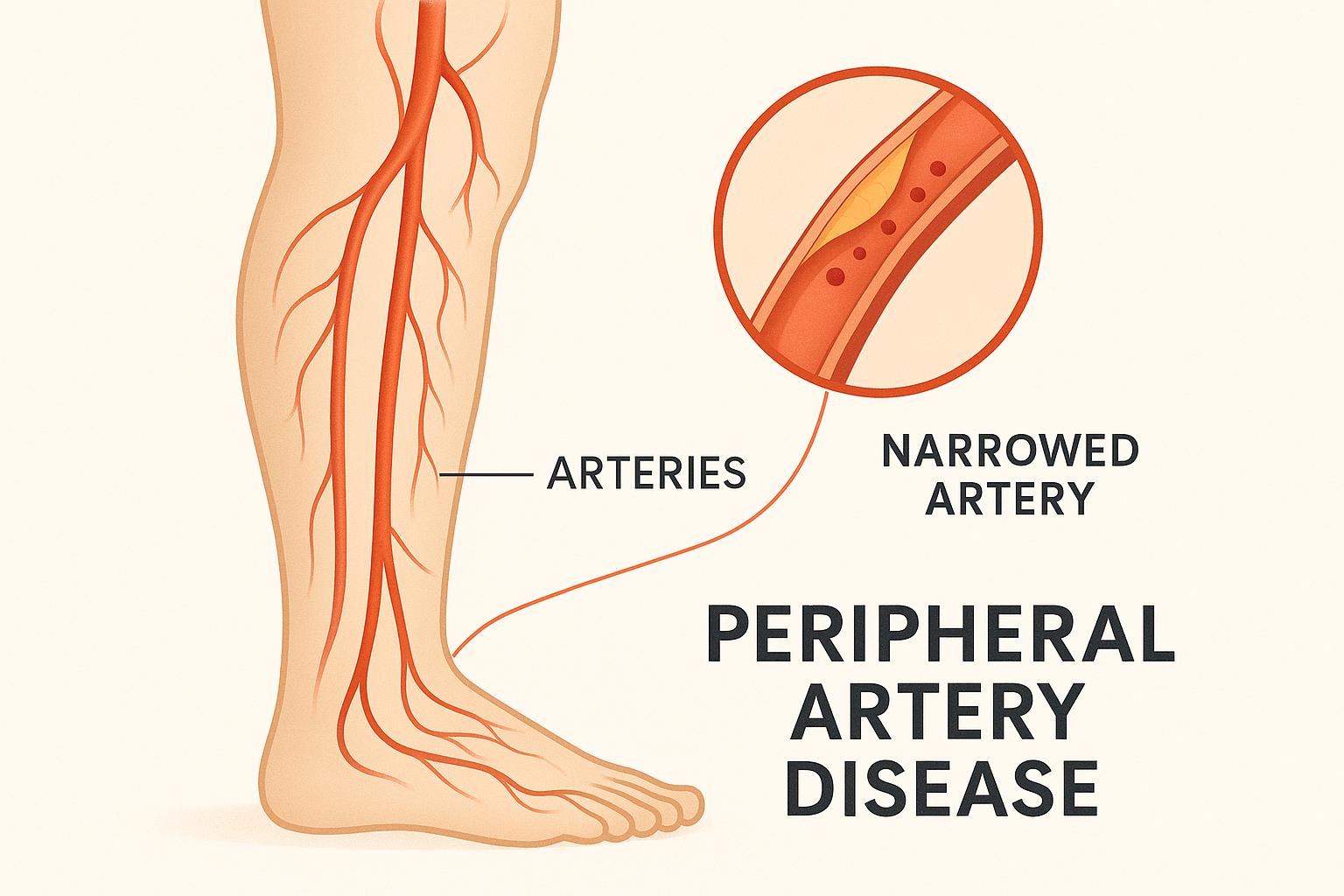
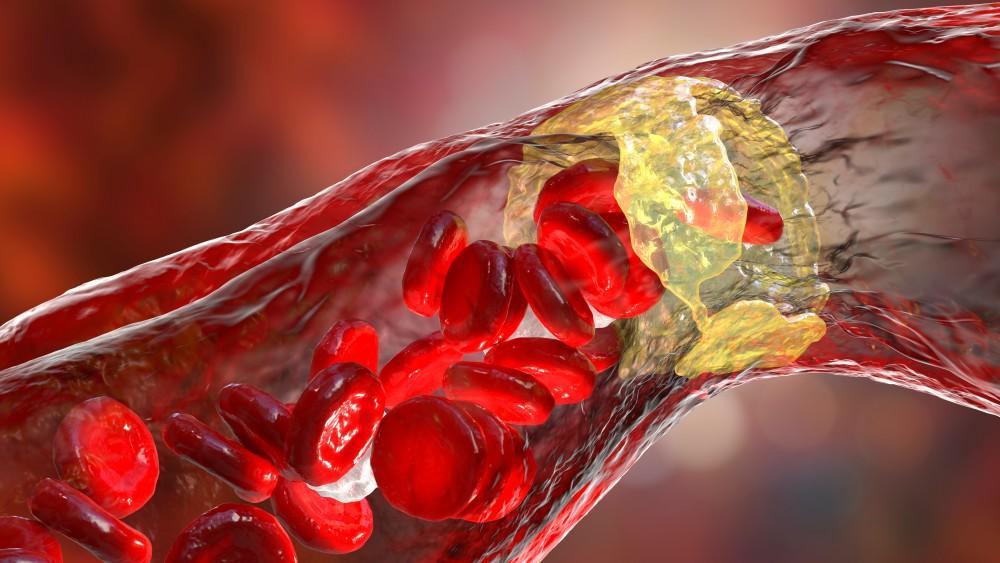
- Hardening of the arteries (atherosclerosis)
- Smoking
- Being male
- Being white
- High blood pressure
- Genetic predisposition
Smoking, though, presents the greatest risk factor for developing an abdominal aortic aneurysm. A study in the December 1999 issue of the Journal of Vascular Surgery found that current smokers were 7.6 times more likely to have an AAA than nonsmokers, while ex-smokers were 3.0 times more likely to have an AAA than nonsmokers. Duration of smoking significantly increased the risk of AAA, with each year increasing the risk by 4%.
Smoking wreaks its havoc by weakening the aortic walls, increasing the possibility not only of developing an aneurysm, but also of causing a dissection.
Genes play a role in thoracic aortic aneurysms, too, and certain conditions, such as Marfan syndrome and Loeys-Dietz syndrome, may also present a risk.
Other causes include:
- High blood pressure
- Infection
- Atherosclerosis
- High cholesterol
- Sudden traumatic injury
How are aortic aneurysms diagnosed and treated?
Because they’re largely asymptomatic, both thoracic and abdominal aneurysms are usually diagnosed when your doctor is examining your abdomen for another reason. If he suspects an aneurysm may be present, he’ll feel your stomach to determine if it’s rigid or contains a pulsing mass or check the blood flow in your legs for an AAA. He also may order an echocardiogram (sound waves that examine the heart) if he suspects a thoracic aneurysm. Other tests he might use include:
- CT or MRI scan
- Ultrasound
- Chest X-ray
The first step in treatment is monitoring, along with lifestyle changes that definitely include stopping smoking if you currently smoke, eating a healthy diet, and getting enough exercise.
If you have high blood pressure, high cholesterol, or blockages in your arteries, your doctor may prescribe medications such as beta blockers or statins to get those under control.
Surgery is always the option of last resort, and if your aneurysm is small, it’s better to monitor and re-test every few months rather than taking on the additional risks that surgery brings. If you do require surgery, Dr. Shah opts for minimally invasive procedures.
Do you think you might be at risk of an aortic aneurysm? Do you want to learn more about what you can do to prevent one? Contact Prime Heart and Vascular to set up a consultation by calling us at 972-295-7017 or by booking your appointment online today.